Rev’s Transcript Library
Explore our extensive collection of free transcripts from political figures and public events. Journalists, students, researchers, and the general public can explore transcripts of speeches, debates, congressional hearings, press conferences, interviews, podcasts, and more.

Marco Rubio Visits India
Secretary of State Marco Rubio and India’s External Affairs Minister Subrahmanyam Jaishankar hold a press conference in New Delhi. Read the transcript here.

“Healthcare Is Human” Rally on Capitol Hill
Actor Noah Wylie speaks at the “Healthcare Is Human” rally on Capitol Hill. Read the transcript here.

Anti-Fraud Efforts in Minnesota Announced
DOJ, RFK Jr., and Dr. Oz unveil record Minnesota Medicaid fraud crackdown. Read the transcript here.

Fed Chair Kevin Warsh's Swearing-In Ceremony
Kevin Warsh is sworn in as the new Fed Chair. Read the transcript here.

EPA Annoucement on Refrigerant Regulations
EPA loosens regulations on refrigerant chemicals to drive down grocery costs. Read the transcript here.

Southern Poverty Law Center Hearing
House Judiciary Committee hearing on allegations against Southern Poverty Law Center. Read the transcript here.
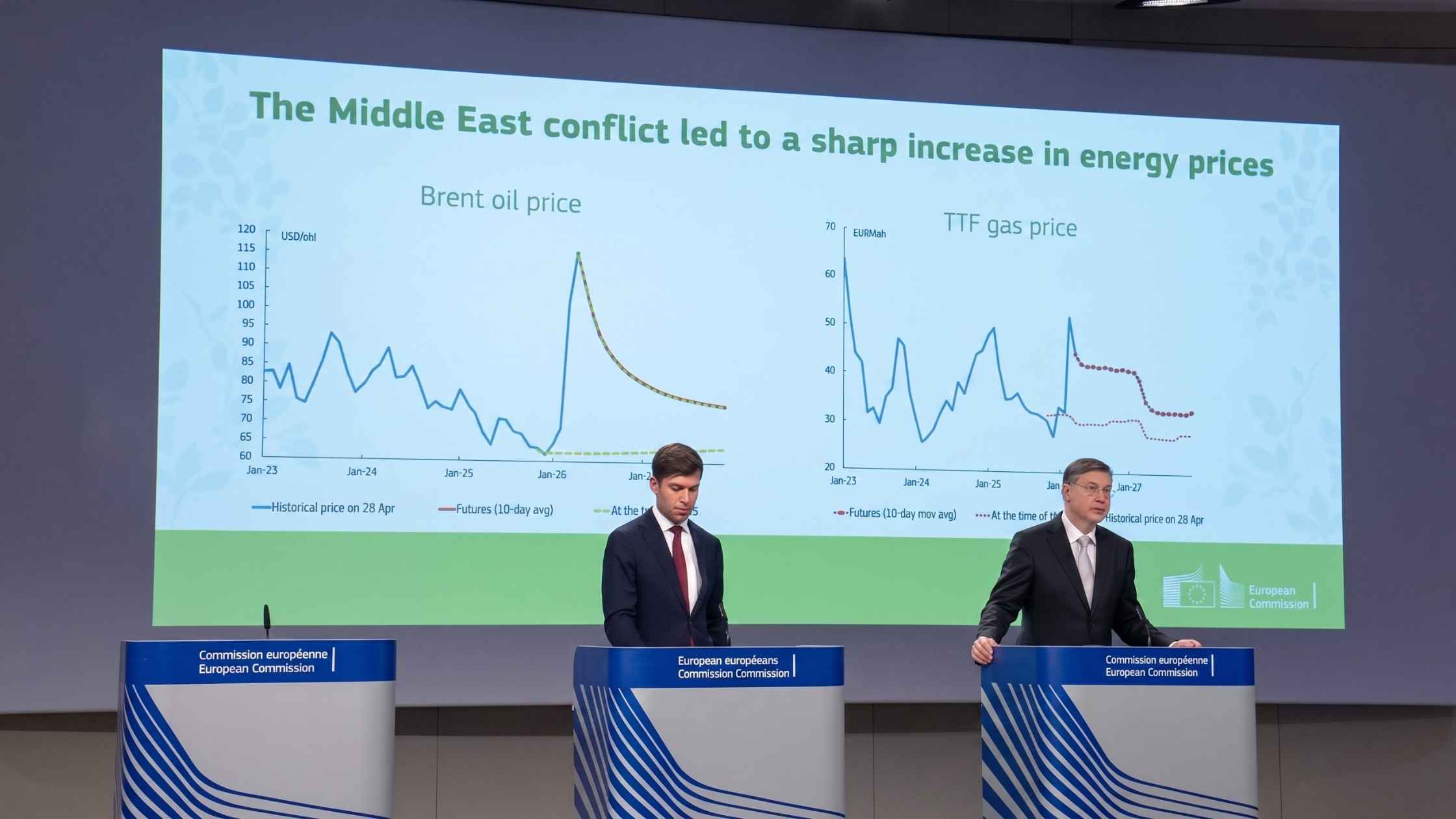
EU Economic Forecasts
EU economy commissioner Valdis Dombrovskis presents the economic forecasts for 27 EU countries. Read the transcript here.

Indictment Of Cuba's Raúl Castro
Acting AG Todd Blanche holds a press briefing to announce the indictment of Raúl Castro in Miami, Florida. Read the transcript here.

U.S. Coast Guard Academy Commencement Address
Donald Trump delivers the U.S. Coast Guard Academy commencement address. Read the transcript here.

CAP Ideas Conference
Democrat leaders speak at the Center for American Progress Ideas Conference. Read the transcript here.

NATO Military Chiefs Hold Press Conference
NATO Military Chiefs hold a press conference following Brussels meeting. Read the transcript here.

DOJ Appropriations Hearing
Acting Attorney General Todd Blanche testifies before the Senate Appropriations Committee. Read the transcript here.
Subscribe to The Rev Blog
Sign up to get Rev content delivered straight to your inbox.
