Rev’s Transcript Library
Explore our extensive collection of free transcripts from political figures and public events. Journalists, students, researchers, and the general public can explore transcripts of speeches, debates, congressional hearings, press conferences, interviews, podcasts, and more.

Federal Reserve and FDIC Hearing
Federal Reserve and FDIC officials testify on financial regulation in a House hearing.

House Agriculture Hearing
Brooke Rollins testifies on USDA priorities in a House Agriculture hearing. Read the transcript here.
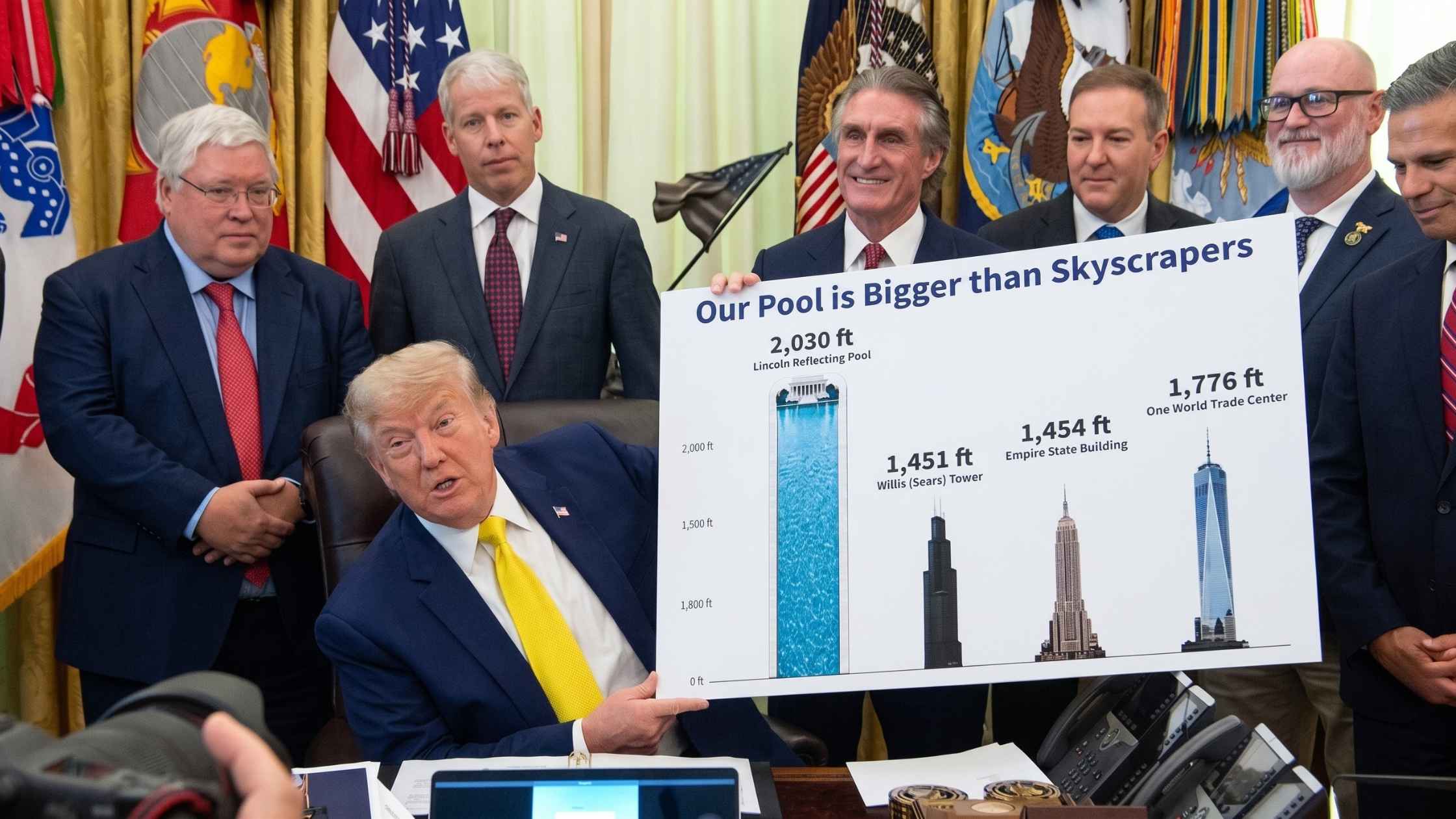
Coal Industry Announcement
Donald Trump makes an announcement about the coal industry in the Oval Office. Read the transcript here.

Senate Finance Committee Hearing
Treasury Secretary Scott Bessent testifies before the Senate Finance Committee. Read the transcript here.

Rubio Testifies Before Senate Foreign Relations Committee
Secretary of State Marco Rubio testifies before the House Foreign Affairs Committee on the State Department's 2027 budget request. Read the transcript here.

DHS 2027 House Budget Hearing
Department of Homeland Security Secretary Markwayne Mullin testifies before the House on 2027 budget request. Read the transcript here.

Senate Forest Service Oversight Hearing
U.S. Forest Service chief testifies in a Senate oversight hearing. Read the transcript here.

State Department Senate Budget Hearing
Marco Rubio testifies before the Senate on the 2027 State Department Budget request. Read the transcript here.

Carney speaks in New York City
Canadian Prime Minister Mark Carney speaks to the Economic Club of New York. Read the transcript here.

FIFA Security Press Conference
FBI officials hold a press conference on FIFA World Cup security in Atlanta, Georgia. Read the transcript here.

Conan O’Brien Gives Harvard Commencement Speech
Conan O’Brien speaks at the Harvard graduation ceremony. Read the transcript here.

White House Briefing 5/28/26
Scott Bessent holds the White House Press Briefing for 5/28/26. Read the transcript here.
Subscribe to The Rev Blog
Sign up to get Rev content delivered straight to your inbox.
