Rev’s Transcript Library
Explore our extensive collection of free transcripts from political figures and public events. Journalists, students, researchers, and the general public can explore transcripts of speeches, debates, congressional hearings, press conferences, interviews, podcasts, and more.

White House Budget Hearing
OMB Director Russell Vought testifies on White House 2027 budget request in a House hearing. Read the transcript here.

Pentagon Press Briefing on 4/26/26
Pete Hegseth delivers the Pentagon Press briefing on the Iran war for 4/16/26. Read the transcript here.

Melania Trump Speaks at Foster Care Meeting
Melania Trump attends a House Ways and Means Committee meeting concerning the foster care system. Read the transcript here.
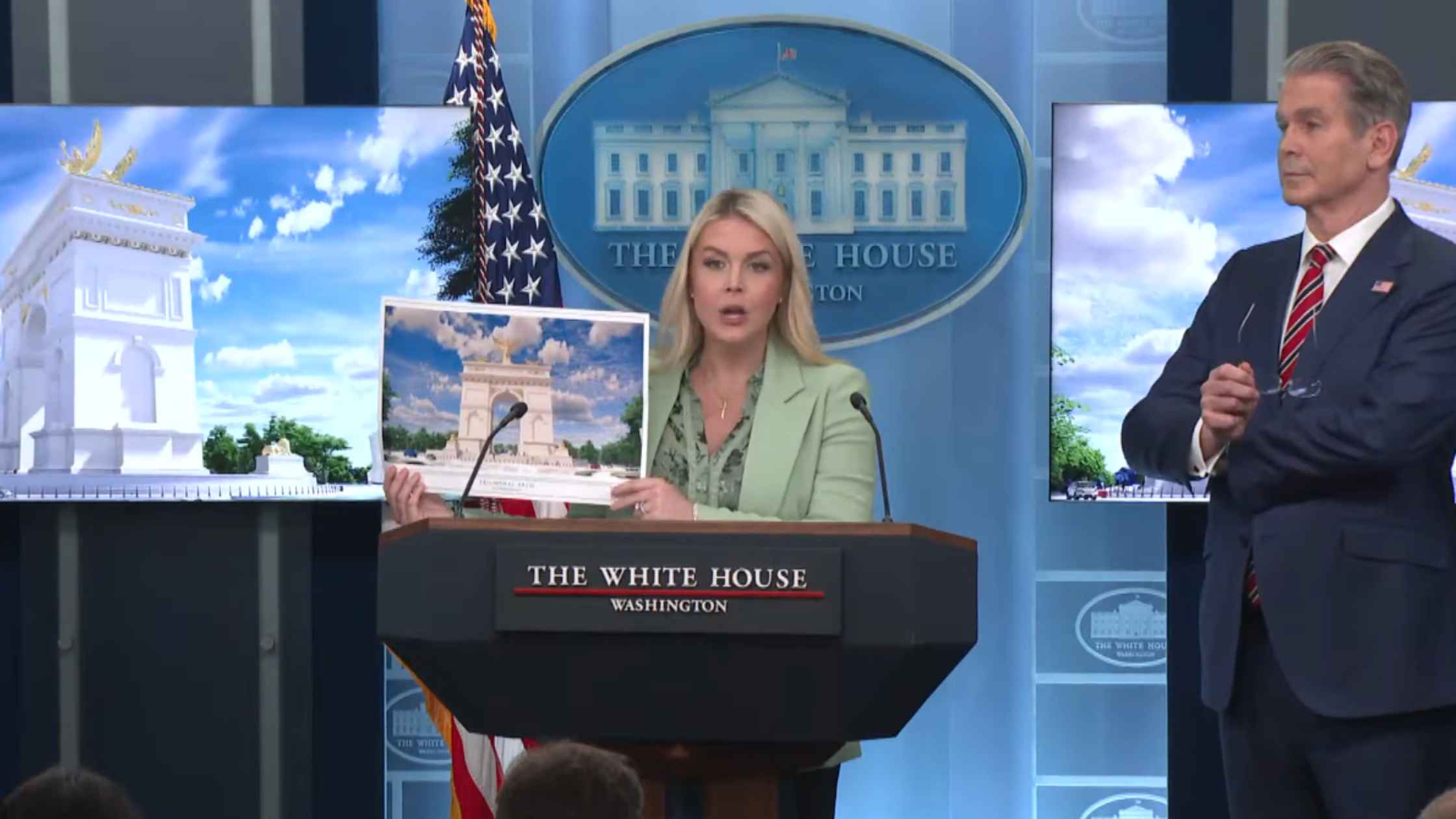
Karoline Leavitt White House Press Briefing on 4/15/26
Karoline Leavitt holds the White House Press Briefing for 4/15/16. Read the transcript here.

UK Parliament on Iran Conflict
British Prime Minister Keir Starmer heads a meeting of the British Parliament focused on the Iran conflict. Read the transcript here.

Carney Press Conference In Ottawa
Canadian Prime Minister Mark Carney holds a news briefing in Ottawa. Read the transcript here.

Vance Speaks at TPUSA Event
J.D. Vance speaks at a Turning Point USA event at the University of Georgia. Read the transcript here.

Swalwell Accuser Holds News Conference
Lonna Drewes holds a press conference detailing her accusations of sexual assault against U.S. Representative Eric Swalwell. Read the transcript here.

Semafor World Economy Forum 2026
Semafor World Economy 2026 summit in Washington, D.C. Read the transcript here.
Subscribe to The Rev Blog
Sign up to get Rev content delivered straight to your inbox.








